My favourite superhero is Robert Downey Jnr’s Ironman / Tony Stark in the Marvel comic book series. But too much iron isn’t such a great thing for humans.
You’re about to learn why too much iron can be a very bad thing.
Based on events this week I wanted to make sure you’re aware of a common genetic disease that can creep up on you without you even knowing it.
This week I received blood test results for a male in his mid thirties who has been experiencing fatigue and lethargy.
He has also blacked out for no apparent reason on more than one occasion and a raft of neurological tests has revealed no obvious cause.
I’m keeping this gentleman’s identity private. Confidentiality is of the utmost importance as this is a sensitive case study and I cannot, for obvious reasons, share his real name.
His blood result this week showed very high levels of two iron markers, ferritin and transferrin saturation, as you can see here:
![]()
When these markers are high and the person eats a balanced diet and has not been having blood transfusions, we have to suspect an iron overload disorder.
My client’s family history, especially that of his brother and father, suggest a hereditary condition may be playing a role in health challenges.
Iron overload, known as hereditary haemochromatosis (HHC) can lead to complications, so it must be taken seriously.
The biggest challenge is that it doesn’t cause any symptoms for many years.
You can go through three, four or even five decades of life without even knowing you have HHC, and then BOOM – you develop a significant problem.
If you have a family history of chronic fatigue, arthritis, liver disease and cardiovascular disease please pay special attention because these can all be caused by iron overload.
The graph paints the picture for you:
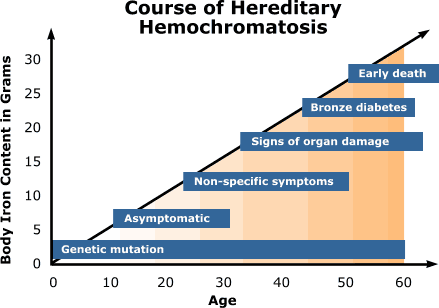
From: http://www.preparemd.com/conditions/iron-overload-disease-hemochromatosis/
What exactly is iron overload disease / HHC?
Frequently we see people with inadequate iron, known as iron deficiency.
This is especially the case in people who have H. pylori because the infection inhibits iron absorption.
But HHC is a different animal altogether – it is a genetic medical condition where gene mutations cause the body absorbs and stores too much iron.
The gene mutations have fancy names, the main ones being HFE c282c and HFE h63d.
While these genes are important, there may be other important ones that contribute to the disease.
Iron overload can also result from blood transfusions and eating a diet high in iron (in which case it is not called HHC).
How many people have iron overload / HHC?
You can inherit the faulty HFE gene from both mum and dad, or from one or the other.
- Homozygous iron overload, where you have two copies of the ‘faulty’ gene (from mum and dad) affect approximately 1 in 250 Caucasians and Hispanics, and 1 in 80 folk with African descent.
- Heterozygous iron overload, where you have only one copy of the faulty gene (from mum or dad) may be as common as 1 in 7 persons!
The condition is more prevalent in the male side of the family rather than the female (recall that my client’s brother and father also have symptoms).
Here’s the important bit: HHC is the most common genetic disease we know of.
But have YOU heard of it?
No?
Me neither until I read a massive 950-page book o inflammation a few years back.
Some experts believe EVERYONE should be tested for HHC, whether we have symptoms or not.
Why?
Because symptoms do not develop until later in life when significant organ damage may have already been done.
I don’t know about you, but feel it is an outrage that every member of society is not informed this condition.
How does iron overload / HHC cause problems?
As iron accumulates in the body it deposits in tissues and becomes toxic.
Excess iron creates inflammation and oxidative stress, which can damage your tissues.
Early symptoms, which may begin in the teens, 20’s or 30’s (like my client with his low energy once he reached his mid 30’s) include:
- Low energy
- Lethargy
- Weakness
- Muscle pain
- Joint pain
- Skin problems
- Weak immune system – increased severity and frequency of infections
- Liver problems
- Neurological symptoms
- Anemia (not iron, but other forms)
- Sudden infant death syndrome
- Alcoholism
- Kidney stones (possible)
Aspects of family history that can point to the condition include:
- Anemia
- Cardiac disorders
- Heart disease
- Arthritis
- Diabetes
- Neurologic disorders
- Liver disease
- Impotence
- Amenorrhoea (no periods)
- Sterility
If diagnosed very late in its progression, or if left untreated, the condition can lead to:
- Diabetes (either type I or type II)
- Cardiovascular disease – palpitations to more serious conditions
- Arthritis and other forms of muscle and joint pain
- Liver cirrhosis
- Hypothyroidism
- Bronzing of the skin
- Testicular failure
- Neurologic disorders (e.g. dementia)
According to one of my teachers, Dr. Alex Vasquez, “The classic presentation is bronzed diabetes with arthritis and cirrhosis.”
How to get tested for iron overload / HHC?
When doctors run blood tests, they often assess iron levels using only one marker or parameter, namely serum iron.
This is inadequate because it does not tell you how much iron is stored in you’re the body.
A full iron panel should include three or four markers:
- Serum iron is a measure of iron in the blood (high levels mean excess iron)
- Serum ferritin is measure of iron storage (high levels mean excess iron)
- Transferrin saturation is the amount of iron attached to transport proteins (high levels mean excess iron)
- Total iron binding capacity is the amount of free storage space (low levels mean excess iron)
Ferritin and transferrin in particular should be assessed as a matter of routine, but are sadly not considered in many cases.
Serum iron is the favoured iron marker, yet it can remain normal despite excessive iron storage.
A blood test with high ferritin and transferrin along with (possibly) low iron binding capacity is a red flag for iron overload.
If these markers are high, additional tests are required to confirm the diagnosis of HHC / iron overload:
- Genetic test for HFE gene mutations (blood or saliva
- The absence of these gene mutations does not rule out HHC because other genes may also be responsible, but we don’t yet know what they are (e.g. research has not uncovered them)
- Liver biopsy
- Liver MRI
Back to my client
My client’s blood test carried other clues that were suggestive of iron overload.
First, he had low insulin, which is very rare (see below):
It may indicate that he has developed some pancreatic damage and this may in turn lead to type I diabetes, a known consequence of haemochromatosis.
This marker is of concern and I have asked him to repeat it with his doctor to confirm accuracy (though I am 99.9% sure it is an accurate result).
Perhaps his blackouts were due to low insulin and a resulting lack of glucose entering his cells (especially the brain cells).
Second, his bilirubin was significantly elevated. The literature shows that bilirubin is often elevated in haemochromatosis, possibly as a defence mechanism.
Third, his white blood cell count was quite low, which again is consistent with haemochromatosis (although it can have other causes).
Finally, his inflammation markers do not appear elevated, which is important because infections and inflammation can cause elevations in ferritin.
Elevated ferritin can result from inflammation
If high ferritin is accompanied by high inflammatory markers such as CRP and ESR, it may be that there is an inflammatory response to, say, an infection.
My client’s inflammation markers did not appear elevated.
While I can’t rule out an inflammatory response as a reason for this elevated ferritin, it remains a possibility.
All in all, however, my client’s health history, symptoms, family history and blood testing strongly suggest haemochromatosis.
Next steps
I referred my client immediately to get the HFE genetic test done. If the test is positive, we can safely assume he has haemochtomatosis.
If they are negative, he can still have the disorder, but we will know it is not genetic.
This is important because we want to know whether the genes may be affecting his brother and father (we also have his three young children to consider as well).
He will also go to his doctor to request a repeat blood test that again checks his insulin and inflammatory markers to rule out any false readings from the original test.
If the insulin level is indeed shown again to be low, he will be referred to an endocrinologist to look for possible diabetes.
I will keep you posted.
Iron overload / HHC summary
- Hereditary iron accumulation disorders occur in a large percentage of the population.
- Persons with the disease usually have no symptoms.
- Clinical manifestations are often indicative of irreversible organ damage or organ failure.
- Iron overload can cause death if not treated early.
- Early treatment ensures normal life expectancy.
Therefore, early detection before the onset of symptoms and organ damage requires screening people BEFORE they have symptoms.
This disorder affects at least one percent of the general population, which is a HUGE number of people.
How you can get tested
It is very wise to rule out iron overload if you have a family history of fatigue, diabetes, arthritis, cardiovascular disease and other conditions mentioned in this article.
Early detection prior to organ damage means that you can manage the condition and live a normal life.
The key blood test markers are:
- Serum ferritin
- Transferrin saturation
If ferritin and transferrin are too high, you must rule out inflammation using these tests:
- ESR (erythrocyte sedimentation rate)
- Hs-CRP (high sensitivity C-reactive protein)
If ESR and CRP are not elevated, there is a chance you have hereditary haemochromatosis (HHC) also known as iron overload.
It needs to be confirmed by genetic testing and liver biopsy or MRI, which your doctor would be able to help you with.
Because the disease creeps up on you over time, it’s wise to have ferritin and transferrin measured every 6-12 (preferably every 6 months).
Need some help?
As always, these are all long words and it can get a little confusing if we’re not careful.
If you’d like some help, we are now offering a service called functional blood chemistry analysis.
Here, we go through your blood test results with you in great detail, looking for patterns and minor/moderate imbalances that may not show up on a regular doctor’s analysis.
We have some software that narrows the reference ranges on your blood work, enabling to spot things that might otherwise be missed.
It helps you head off problems at the pass, so to speak and it will give you clues about why you might not be feeling well.
You can either get the blood test done with a doctor and send us the results, OR we can arrange the testing for you (U.K., U.S., Canada) via our affiliate labs.
You can learn more about functional blood chemistry analysis here.
Oh, and whatever happens, I’ll also keep you posted about my client’s genetic testing.
Best,
Dave.

Comments are closed.